1. Name of the location of 90% of epistaxis
2. A genetic disorder that forms AV malformations in the skin, lungs, brain etc
3. Name of posterior vascular plexus in the nasal cavity causing posterior epistaxis
4. 1st line treatment for all epistaxis
5. The common brand name for anterior nasal packing
6. Chemical used in cautery sticks
7. Physically scaring complication of posterior nasal packing with foleys catheter
Coming soon..
Acute Otitis Media
Introduction
This can be defined as an inflammatory condition of the middle ear cleft. There are several subtypes and the important ones for this course are: acute otitis media, otitis media with effusion (sometimes called glue ear), chronic suppurative otitis media (perforations and cholesteatoma).
Acute Otitis Media
This is common in children and is viral or bacterial. Viral forms are usually brief while bacterial forms may last days.
Symptoms
-
Often there is a preceding viral URTI (e.g. rhinovirus or adenovirus)
-
Earache/pain. Often throbbing and may be severe
-
Constitutional symptoms – malaise, pyrexia
-
Hearing loss
-
Pain increases as pressure builds behind the tympanic membrane. If bacterial, pus may burst through the ear drum. If it does, the pain resolves and there is yellow discharge from the ear canal
Signs
In un-complicated cases:
-
Mild fever
-
Red drum or bulging of the drum (see images below)
-
Distress
-
Mucopurulent discharge may be seen if the drum has ruptured

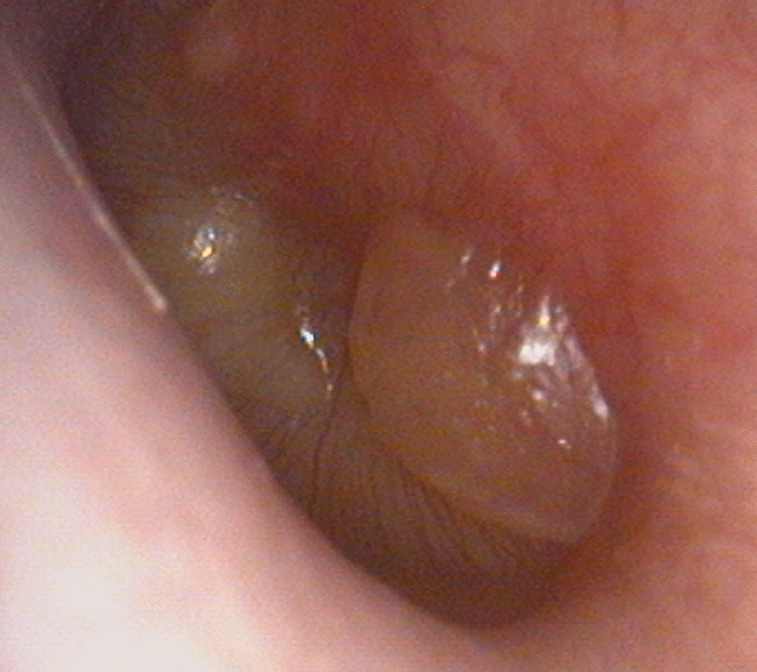
Management
In un-complicated cases:
-
Pain relief is usually all that is required as the condition is usually brief
-
Oral antibiotics e.g. amoxicillin if the condition persists for three days or more or if the child is under 2 years of age. This applies whether or not there is aural discharge
-
Treatment of underlying otitis media with effusion if this is persistent
OE picture
Complications / red flag symptoms
-
Temperature / sepsis
-
Sub-periosteal mastoid abscess
-
Cranial nerve palsy
-
Symptoms of meningism
-
Altered conscious state
-
Labyrinthitis
-
Extradural or parenchymal brain abscess
-
Abscess in the neck
Management of complications
Any sign of complications of OM:
All of these patients should be admitted and the ENT team on-call be made aware as soon as possible
-
Adopt the ALS principles with an ABCDE approach and perform a thorough examination
-
Will require IV Antibiotics (as per local antibiotic usage guidelines), fluid if shocked, analgesia and complete set of bloods, swab ears
-
Keep NBM until reviewed by SpR or consultant
-
Definitive management should be guided by the SpR on-call e.g. may require CT scan, surgery (myringotomy, abscess drainage)
For more information on antibiotic use in AOM, please see our antibiotics section.
Subperiosteal Mastoid Abscess - often mistakenly called 'mastoiditis'
This is one of the commoner complications of otitis media. You will find it referred to as 'mastoiditis' but this is an incorrect and lazy appellation. Mastoiditis, or inflammation of the mastoid mucosa, is an inevitable accompaniment to otitis media. Indeed, otitis media means 'inflammation of the middle ear cleft' of which the mastoid is a part.
The patient is almost always a young child, presents with a very typical appearance: the pinna is pushed forwards and downwards, there is a red swelling behind the pinna overlying the mastoid bone, and that swelling is fluctuant. There is often a fever and the ear canal may be swollen. The drum, if seen, will show signs of acute otitis media as described above.
All of these patients should be admitted and the ENT team on-call be made aware as soon as possible
-
Adopt the ALS principles with an ABCDE approach and perform a thorough examination
-
Will require IV Antibiotics (determined by local antibiotic stewardship guidelines), fluid if shocked, analgesia and complete set of bloods, swab ears
-
The antibiotics should cover the usual bacteria that cause acute otitis media
-
Keep NBM until reviewed by SpR or consultant
-
Definitive management should be guided by the SpR on-call. This will usually include 24 hours of antibiotics and then a myringotomy and grommet insertion plus drainage of the abscess behind the ear via a cortical mastoidectom..

