1. Name of the location of 90% of epistaxis
2. A genetic disorder that forms AV malformations in the skin, lungs, brain etc
3. Name of posterior vascular plexus in the nasal cavity causing posterior epistaxis
4. 1st line treatment for all epistaxis
5. The common brand name for anterior nasal packing
6. Chemical used in cautery sticks
7. Physically scaring complication of posterior nasal packing with foleys catheter
Coming soon..
Otitis Externa
Definition
Acute inflammation/infection of the skin of the external auditory canal. It can be diffuse (affecting the whole canal) or localised (furuncle – may need lancing). approximately 10% of people can expect an episode of this in ther lifetime.
Aetiology
Bacterial, fungal, rarely viral. Water exposure, dermatological predisposition e.g eczema, trauma to skin
from scratching or cotton buds, and relatively high environmental humidty are all risk factors.
Symptoms
There is a history of increasing otalgia (worse on moving pinna or tragus) with or without:
-
Thick ear discharge
-
Conductive hearing loss
-
Tinnitus
-
Dizziness or disequilibrium (sometimes true vertigo)
-
Swelling of pinna/face
Clinical Findings
-
Oedema
-
Erythema
-
Stenosis of the ear canal
-
Debris/discharge
Profuse muco-purulent discharge is usually indicative of middle ear disease.
Appearances of otitis externa
The pictures below show a patient with diffuse otitis externa. We see the first signs of otitis externa with otorrhoea from the external canal. Click figure 1 to see a magnified view of the canal. Finally, otoscopy confirms the diagnoses of an otitis externa with a large amount of debris & discharge (figure 2).
Click the image to magnify
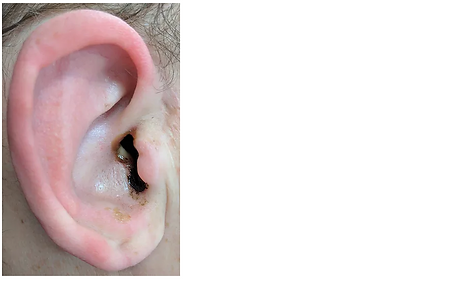



Figure 1 otorrhoea in the external canal
Figure 2 otitis externa on otoscopy
Who should be referred to Secondary care?
The following scoring system helps identify which patients can be managed in the community, which patients need to be seen by ENT, and how urgently they need to be seen.

Management
Treatment: (See ABMU dept protocol)
1. Aural toilet. Performed with a microscope and microsuction or mopping with cotton wool (often kinder/ less distressing in children). Thorough explanation to the patient of what microsuction entails is good practice. It is “Loud” and can be uncomfortable
2. Antibiotic treatment. Topical antibiotic treatment e.g. ciprofloxacin, neomycin or gentamicin in the form of drops is usually required. Oral antibiotics are not used in OE unless the skin infections spread outside the ear canal onto the pinna or face.
3. Insertion of a Pope wick. Acute oedema and stenosis of the EAC often require insertion of a wick to ensure treatment reaches the full extent of the affected canal.
Insert with care (the wick is hard before antibiotic drops are placed), ensure you follow the line of the ear canal. Apply antibiotic immediately after insertion to soften and expand the wick. Prescribe ear drops as normally and arrange for removal of the wick after 48 hours.
4. Water precautions and advice should be given. Leaflets are available in the department for patients to read.

For more information on different ear drops please see our topical antibiotics section.
Complications of otitis externa can include pinna cellulitis and canal stenosis. Cellulitis usually requires oral antibiotics (or IV if it spreads widely or on to the face).
Malignant Otitis Externa (MOE)
This is the commonly used name for the condition 'necrotising otitis externa'. MOE is an infection of the skin of the outer ear that spreads to affect the tympanic bone at the bony-cartilaginous junction of the floor of the ear canal.
From this, osteomyelitis spreads medially through the bone to include the skull base and damages cranial nerves as it does so.
The infecting pathogen is almost always Pseudomonas aeruginosa.
There are a number of features that are typical:
1. Age. This is generally a disease of the elderly
2. Immunity. It is commoner in immunocompromised patients. Elderly diabetics make up the majority of cases but patients on chemotherapy or who have other disease-causing depressed immunity are vulnerable
3. Pain is a key feature. The patient is in disproportionate pain to the clinical appearance of the ear canal
4. Aural polyp. This is a common feature. It is situated at the bony-cartilaginous junction of the floor of the ear canal.
5. Cranial nerve palsy. As the disease spreads medially it causes cranial nerve palsies. A lower motor neurone VII palsy is the commonest of these and is a red flag sign in OE. Other lower cranial nerves can be affected once the infection reaches other skull base foramina and may cause difficulty with swallowing or speech.
Management of MOE
Diagnosis is achieved by history and examination supplemented with CT of the skull base and microbiology
from a swab of the ear discharge. Biopsy of the polyp in the ear canal is often performed to rule out malignancy. Radionucleotide scans are rarely performed. MRI may be required if intracranial spread is suspected.
Medical management depends upon sensitivities of the orgnaisms and whether the patient is allergic to penicillin. The choice of antibiotic is often directed by the microbiology department and may include drugs such as Piperocillin with Tazobactam, Meropenem, or Ciprofloxacin. Up to six weeks of therapy may be needed in some cases. In all cases, topical antibiotics, such as gentamicin, are used to control the infection within the ear canal skin.
Control of diabetes is important and so is the management of pain.
Surgery is not routinely performed.

