1. Name of the location of 90% of epistaxis
2. A genetic disorder that forms AV malformations in the skin, lungs, brain etc
3. Name of posterior vascular plexus in the nasal cavity causing posterior epistaxis
4. 1st line treatment for all epistaxis
5. The common brand name for anterior nasal packing
6. Chemical used in cautery sticks
7. Physically scaring complication of posterior nasal packing with foleys catheter
Coming soon..
Chronic Otitis Media - Cholesteatoma and Perforations
Introduction
Chronic otitis media is subdivided into cholesteatoma and perforations. This page looks at both of these.
Cholesteatoma
Cholesteatoma is sometimes described as 'skin in the middle ear'. This disease is a form of otitis media characterised by in-growth of skin into the middle ear where it is destructive to middle ear bones and other structures. A list of the parts it can affect is found in the 'Complications' section below.
Types and Aetiology
There are a number of different types of cholesteatoma and these are listed below. You should be familiar with acquired cholesteatoma in particular as it is the most common form and the one you are likely to be examined upon.
1. Congenital cholesteatoma.
This is uncommon and arises in ears that have not been troubled by otitis in the past. It is believed that it grows from a small nidus of epidermal cells that appears in the first trimester of intrauterine life and then fails to regress.
2. Acquired
a. Primary acquired. This is associated with a defect in the pars flaccida.
b. Secondary acquired. Associated with a defect in the pars tensa
c. Tertiary acquired. Arising behind an intact tympanic membrane after previous ear surgery has implanted epithelium into the middle ear e.g. after grommet insertion.
The incidence of acquired cholesteatoma is 1:10,000.
The simplest (and most credible) theory as to the origins of acquired cholesteatoma requires two pieces of knowledge before it can be understood. The first is about epithelial migration and the second about the effect of negative middle ear pressure on various parts of the ear drum.
Epithelial migration
Consider the sequence of images below. In the first an ink spot is seen on the umbo. The second and third images show the same ear three and five days later. The skin of the ear drum and canal all originates from the region of the umbo and then migrates radially in all directions across the drum and out into the canal.

By the time it reaches the external meatus it is ready to die (apoptosis). If the skin of the ear did not behave in this way the ear canal would quickly fill with dead skin.
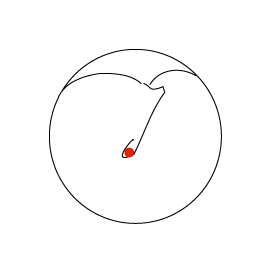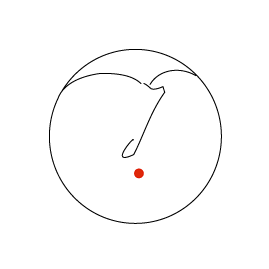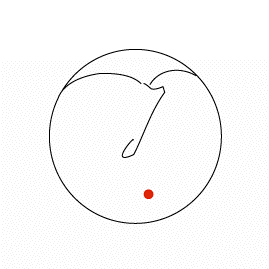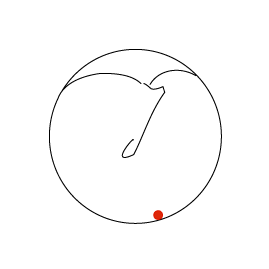
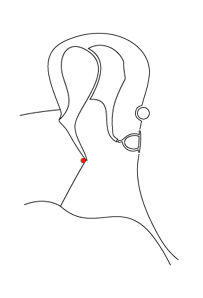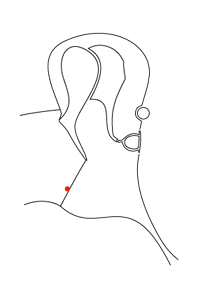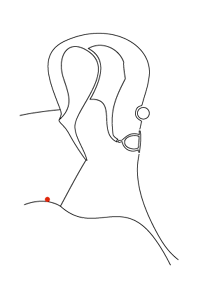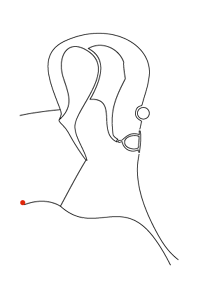
The first animation shows this process as seen from lateral to the drum (the view one normally sees with an auriscope). The second shows it in the coronal plain and follows the red ink spot beyond the drum and towards the external auditory meatus.
Negative middle ear pressure
There are two areas of the ear drum that are weaker than the others: the pars flaccida and the postero-superior quadrant of the pars tensa. When they are subject to continual negative middle ear pressure they become sucked inwards. As time passes this indrawn area can become large enough to deserve the name retraction or 'pocket'. The image below shows this process.
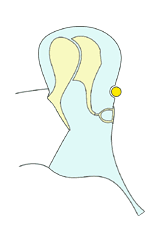
1
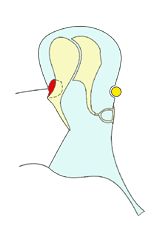
2
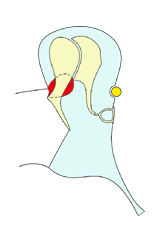
3

4

5
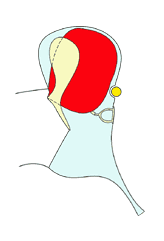
6
When the pocket is small (2) epithelial migration caries skin into and then out of the pocket. The deeper the pocket becomes, however, the harder it is for the skin to move back out of the pocket. Eventually, it is unable to escape at all as when the pocket is large (6).
The image above shows this process of enlargement as seen in the coronal plain. The next images view it as seen from laterally looking inwards towards the ear drum.


1
4
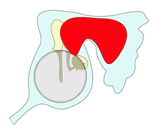
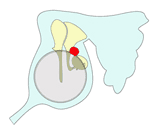
2
5
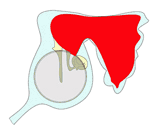
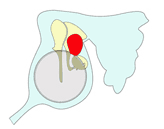
3
6
The cholesteatoma (here shown in red) typically enlarges posteriorly to fill the mastoid but it may also enlarge anteriorly and inferiorly to fill the middle ear cleft. Note how it destroys the ossicles as it enlarges.
Symptoms and signs
Symptoms originate both from the disease and from it's complications (see below). Discharge is classically scanty, green and foul smelling. Pain is notably absent.
Examination of the ear reveals a variety of appearances: there may be a 'crust' in the attic region, a marginal perforation or a pocket of invading keratin. Should active infection be present within the rich keratin medium of the cholesteatoma then pus or aural polyps may be present.

Here is an attic retraction.
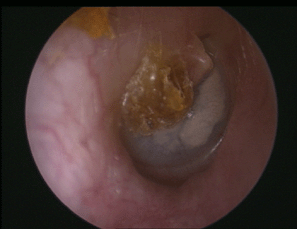
In this ear there is a crust over the postero-superior part of the ear drum and the adjacent attic. Beneath this is a cholesteatoma.
Here you can see keratin (pearly white) associated with aural polyp (granular and red) and pus. All of this is arising from the attic region.
Complications
If the disease is left without treatment or presents late, complications may arise. Please note that this list of complications is similar to that for the complications of acute suppurative otitis media and broadly similar to that for major ear surgery.
When memorising this list you may find it convenient to group the complications in terms of the local anatomy. This is how they are laid out here.
Middle ear complications:
1. Conductive hearing loss as the ossicles are eroded
2. Facial palsy as the bone covering the facial nerve is destroyed
Inner ear complications (medial to the middle ear)
1.Sensorineural hearing loss
2.Vertigo
3.Labyrinthitis
4.Petrositis or inflammation of the petrous temporal bone
Mastoid and posterior fossa complications (posterior to the middle ear)
1.Mastoiditis with subperiosteal abscess (behind the ear).
2.Meningitis
3.Cerebellar abscess
4.Sigmoid sinus thrombosis
Middle fossa complications (superior to middle ear)
1.Meningitis
2.Temporal lobe abscess
3.Extradural abscess
4.Subdural abscess (uncommon)
Anterior and inferior to the ear
1.Abscesses can form in the sternocleidomastoid or in the zygomatic region
Management
Management of cholesteatoma is usually surgical although some patients are not fit for surgery or decline it.
There are many types of operation used to explore the ear and remove cholesteatoma but an understanding of all of these is outside your curriculum. However, you should remember these three operations as they are amongst the commonest:
1. Atticotomy. Used when the disease is limited to the attic region i.e. is relatively small
2. Modified radical mastoidectomy. Used when the disease extends backwards into the mastoid system. It is a more traditional procedure and is being replaced, by many surgeons, with...
3. Combined approach tympanotomy (CAT). Increasingly performed for larger diseases.
All types of surgery are increasingly using rigid endoscopes to facilitate removal of disease and atticotomy can be done entirely with an endoscope in well trained hands.
Surgery has many hazards. There are the risks of surgery in general and risks specific to the operation. The important complications of cholesteatoma surgery to remember are:
1. Facial paralysis - temporary or permanent
2. Worsening of hearing loss or even dead ear
3. Taste disturbance - because the corda tympani travels through the middle ear and may be damaged
during surgery. This is fairly common.
4. Recurring discharge after surgery. This is due to failure of the ear to heal or recurrence of the original disease
Perforations
A perforation is a hole in the eardrum. It is usually caused when an infection in the middle ear bursts out through the drum and the drum does not heal afterwards. This is particularly likely if the eardrum is already thin due to the presence of middle ear fluid (e.g. glue ear in children) or if the Eustachian tube doesn’t work well and there is longstanding negative middle ear pressure.



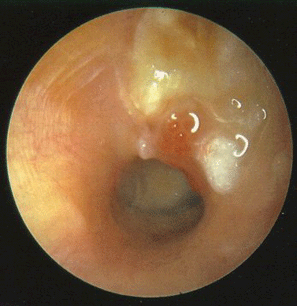
Above are examples of perforations of the eardrum in right ears. The first two are anterior, central perforations while the last is posterior and marginal. In addition the last image shows the head of the stapes very well, an attenuated long process of the incus, the stapedius tendon, and the round window niche.
Symptoms
Some perforations cause no problems and the patient doesn’t know that they have one. However, other patients suffer with recurring discharge and loss of hearing due to the perforation. Very occasionally a perforation will also lead to cholesteatoma. Perforations can be complicated by meningitis and brain abscess.
Infections
The presence of a hole in the eardrum may allow bacteria laden water to get into the middle ear. This will cause an infection which will produce a discharge that may be yellow, green or blood stained. The discharge is sometimes of a high volume.
Another way in which the ear may discharge is following an upper respiratory infection.
Patients who have a perforation must be instructed to keep their ears dry. This may mean avoiding swimming and taking care during bathing and hair washing.
Hearing loss
Patients with a perforation often have hearing loss as well. This is usually a conductive hearing loss and is caused by loss of surface area of the drum. Remember that the size of the drum compared with the oval window is the main way that the ear amplifies sound.
Another reason is that infections that caused the perforation will sometimes damage the ossicles as well. This is particularly a problem for the incus and the incudo-stapedial joint and is more common when the perforation is situated in the posterior half of the drum.
Discomfort, dizziness and tinnitus
These are all possible in perforations especially when there is an infection present. Pain is not usually severe. Any middle ear infection that is associated with vertigo must be treated very seriously and referred to the hospital without delay. Tinnitus is possible in the presence of a perforation whether it is infected or not.
Treatment
Medical treatment is divided into preventative management and treatment of an acute infection. Surgical treatments are also possible.
The presence of a perforation means that the patient is more likely to get infections in the ear. It is important to tell them that they must keep their ears dry. This is difficult when the patient is a child. Water can get in the ear during swimming, using a shower or while taking a bath. Putting something into the ear during these activities can prevent infection from occurring.
Treating the infection when it is present usually fairly easy. Topical medications such as Gentisone HC or Sofradex have been safely used for decades. These days non-ototoxic alternatives exist in the form of quinolone drops.
Myringoplasty
Myringoplasty is an operation to repair the eardrum. It is the simplest type of a wider range of operations known as tympanoplasty. Tympanoplasty comes in a number of different types that involve repair of perforations and rebuilding a route for sound to enter the inner ear by recreating the ossicular chain. Follow this link to the myringoplasty page.

