1. Name of the location of 90% of epistaxis
2. A genetic disorder that forms AV malformations in the skin, lungs, brain etc
3. Name of posterior vascular plexus in the nasal cavity causing posterior epistaxis
4. 1st line treatment for all epistaxis
5. The common brand name for anterior nasal packing
6. Chemical used in cautery sticks
7. Physically scaring complication of posterior nasal packing with foleys catheter
Coming soon..
Vestibular Compensation
Remit
So far, tutorials have concerned themselves with clinical diseases that cause balance upset and have concentrated on the ear itself without consideration of what happens in the brainstem and cerebellum after one of these diseases manifests itself.
This page provides an introduction to the process called 'compensation' that occurs after acute vestibular failure. It starts with a discussion of the immediate effects that loss of vestibular input has on the brainstem, including both static and dynamic effects on the patient, and finishes with the process of compensation itself.
Of necessity it looks in greater detail at the anatomy and physiology of equilibrium, and eye movement.
Where does information from the vestibular nerves go?
Vestibular nerves feed into the vestibular nuclei in the floor of the fourth ventricle of the brainstem. The vestibular nuclei are rather badly named, however, as they dont only receive input from the vestibular nerves. In truth they are sensory integration nuclei receiving input from the ears, eyes, and from proprioceptive sensors. They are linked with the cerebellum and one of their fundamental purposes is to integrate all of the inputs with the aim of maintaining gaze stability.
Vestibular Nuclei
Each vestibular nucleus is really four nuclei in a cluster and these are named according to their position:
Superior vestibular nucleus - the most superior of the four, that is, nearest the nose
Medial vestibular nucleus - nearest the midline
Lateral vestibular nucleus - furthest from the midline and between the superior nucleus and the dorsal nucleus
Dorsal vestibular nucleus - nearest to the feet
Each of these nuclei receives information from a different part of the vestibular apparatus as indicated in the diagram. Information from the semicircular canals goes mostly to the superior and medial vestibular nuclei and these nuclei, in turn, mostly connect with centres higher in the brainstem responsible for eye movement.
The utricle and saccule mostly connect with the lateral and dorsal vestibular nuclei which in turn project down the brainstem towards the spinal cord and centres that move the lower limbs and trunk. Remember that this is a simplification!
The four nuclei communicate with one another and with the nuclei on the other side of the brainstem through a structure called the commissure.
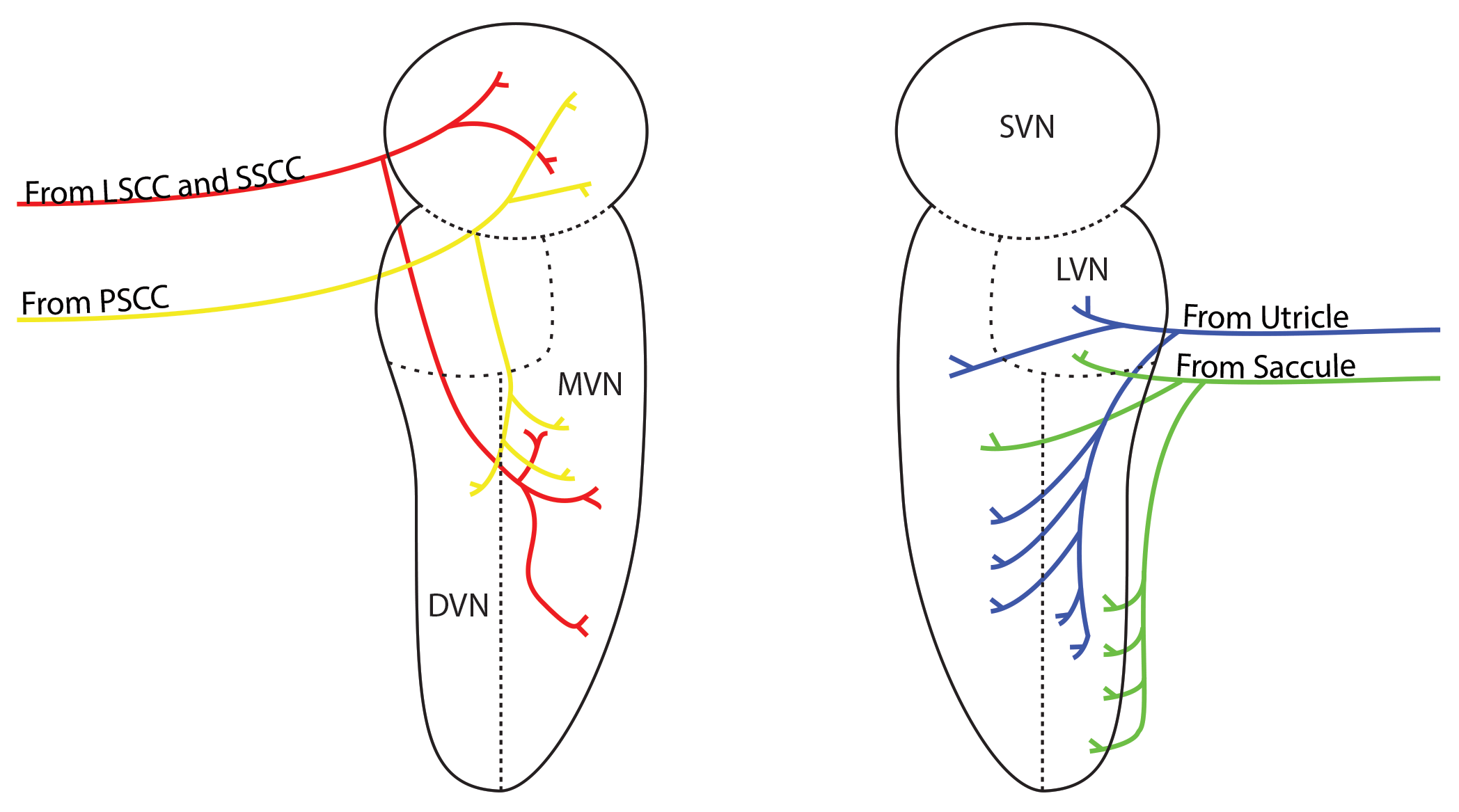
The commissural system
A commissure is simply a collection of neurones that crosses the midline of the brain allowing one side to talk with the other. In the case of the vestibular nuclei this means that the two sides do not work independently of each other. Instead they communicate with each other and modify what each other is doing.
In the vestibular system the influence that each has on the other is inhibitory, that is, one side inhibits the other side's activity. We shall look only at the activity of the medial vestibular nuclei for simplicity and, for further simplicity, only think about inputs from the lateral semicircular canal into the medial nucleus. These are the ones involved in turning the head from side-to-side.
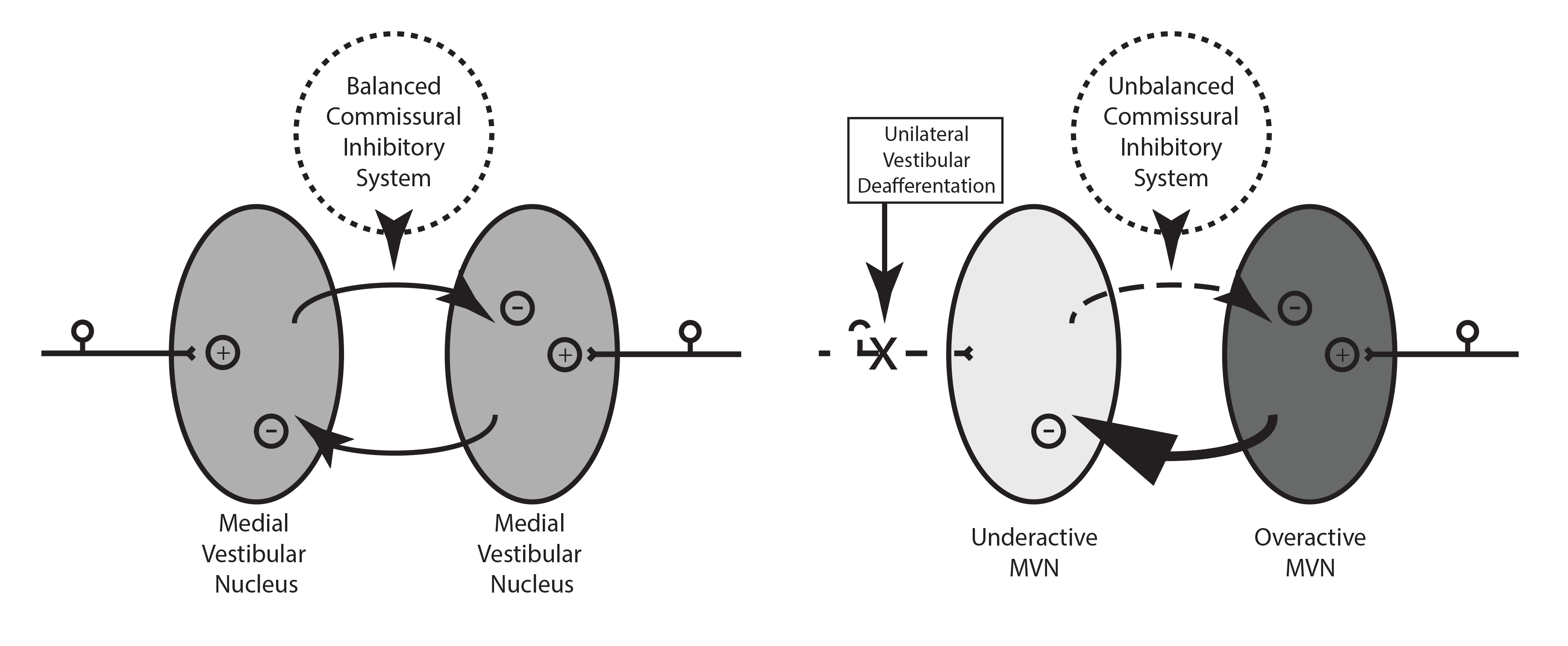
You can see from the diagram that, when there is no head movement and the vestibular nerve activity is equal, the inhibitory activity from one nucleus balances the activity from the other. Both have equal activity.
However, when one of the vestibular nerves increases its activity, such as during a left head turn, the inhibitory activity from the left nucleus also increases (gets darker in the illustration above) and the right nucleus activity is pushed downwards (gets paler).
This has the effect of amplifying the difference in activity between the two nuclei - one already has higher activity because its input has risen and it pushes the opposite side's activity down even further by inhibiting it.
Immediate changes after vestibular failure e.g. in vestibular neuritis
As before we will concentrate only on the activity of nerve fibres coming from the lateral semicircular canal through the superior vestibular nerve. Sensory nerves are afferent nerves. This means that the information that they convey is travelling towards the brainstem. When a sensory nerve is cut or damaged by disease, the term 'deafferentation' is used. In vestibular neuritis, for example, the term 'vestibular deafferentation' (VD) is applied because the vestibular organ is disconnected from the brainstem. In this tutorial we will only be discussion deafferentation from one side (unilateral) - uVD.
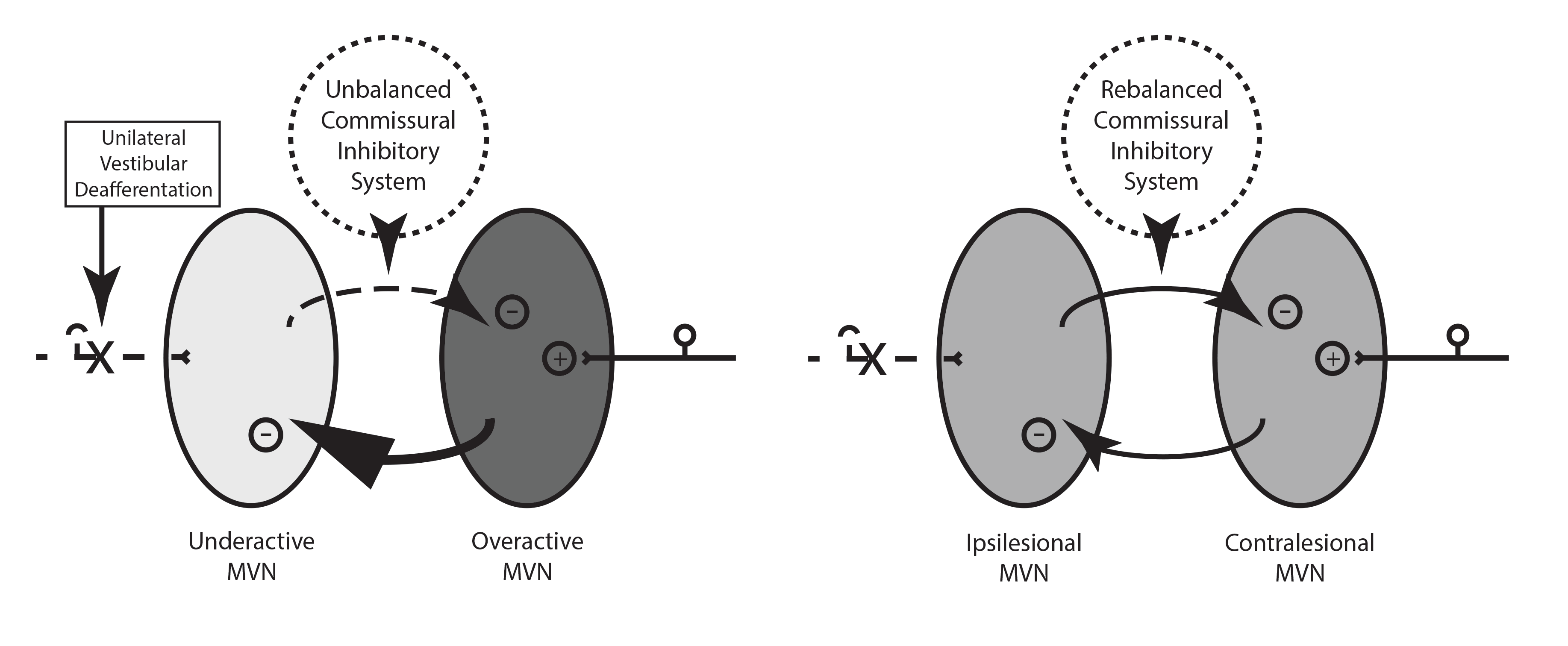
When uVD occurs one vestibular nucleus loses its input and its activity levels fall. However, the other vestibular nucleus is working at normal rate so it inhibits the weak nucleus further, even when there is no movement of the head.
This is an inevitable consequence of the inhibitory commissural system. The asymmetry between the two sides rises further.
It is this asymmetry that is responsible for the acute signs of uVD - nystagmus, ocular tilt reaction, effects on VOR gain and vestibulo-spinal tone.
Clinically, these signs are broken down into two groups: those present while the patient is stationary, and those present when the patient moves.
Static Deficits
Present while the patient is immobile-
Nystagmus
Ocular tilt reaction
Dynamic Deficits
Present while the patient is moving-
VOR loss of gain
Vestibulo-spinal tone
Nystagmus is by far the most obvious static deficit and will be looked at in more detail here.
Nystagmus
Nystagmus is defined as a disorder of ocular posture. Ocular posture is a strange term but it is an important one. We are used to thinking of posture as being the shape of our body in relation to gravity but the eye has posture too. Its position in the orbit must be maintained strictly in order that it can be moved in any direction quickly and accurately and at the same time as the other eye. We dont want it swivelling around when we move or tipping downwards under the influence of gravity.
Posture is maintained by six muscles that act in pairs opposing each other. These muscles are in a continuous state of mild contraction and the effect is to hold the eye looking straight forward in a neutral position. Moving the eye voluntarily or automatically requires one of the pairs of muscles to contract and the other to relax at the same time. For example, if we wish to look sideways to the right we must contract the muscle that turns the eye to the right and relax the muscle that turns the eye to the left.
(Moving the eyes to the right - For the right eye this means contraction of the lateral rectus and relaxation of the medial rectus. For the left eye it means contraction of the medial rectus and relaxation of the lateral rectus. Each of these muscular activities is simultaneous and the eyes move at the same speed, to the same distance, and to the same side.
Nystagmus, sometimes called jerk nystagmus to differentiate it from other involuntary eye movements, has a slow phase and a fast phase. The slow phase is where the eyes drift from their point of gaze, the fast phase is where the eyes snap back to the direction they were looking before they drifted.
Nystagmus is defined by its fast phase. This means that, if the eyes drift to the right and then snap back to the left, it is a left-beating nystagmus.
In ear disease, the eyes drift towards the under-active ear and the eyes snap away from the under-active ear.
The nystagmus of vestibular disease is unidirectional and obeys Alexander's law.
This is a fundamental fact and should be committed to memory, but what does it mean?
A unidirectional nystagmus is one that is always in the same direction regardless of where the patient is looking. So, if it is a left-beating nystagmus it will be left-beating when the patient is looking left, right, up or down.
Another fundamental rule of nystagmus from ear disease is that it obeys Alexander's law. Alexander's law states that, in nystagmus from ear causes, the nystagmus will be worse when the patient looks in the direction of the fast phase and better when they look in the direction of the slow phase.
The video below shows Alexander's law in action in a patient with left-beating nystagmus.
https://www.youtube.com/watch?v=WJGFRTcgbOw
Ocular tilt reaction
In health, when one tilts ones head to one side, the eyes make a compensatory tilt in the opposite direction. This is a utricular reflex. So a left head tilt (ear to shoulder) decreases the activity in the right nucleus and increases the activity in the left nucleus and the eye rolls to the right side to try to maintain a normal visual vertical.
In deafferentation, say on the right, the right activity is driven downwards and this mimics the normal situation during left head tilt. The eyes roll to the right side.
At about a week after a vestibular loss the tilt is about 10 degrees. A month later, as compensation takes place, it is about 5 degrees.
In clinical practice we do not routinely look for ocular tilt reaction but there are some inventive ways of seeing it. These include the bucket test and variants of it. These can reliably detect small changes in the subjective vertical and diagnose vestibular disease. Have a look at the article below for more information.
Brodsky J; et al. Peripheral vestibular loss detected in pediatric patients using a smartphone-based test of the subjective visual vertical. Int J Pediatr Otorhinolaryngol 2015, http://dx.doi.org/10.1016/j.ijporl.2015.09.020
Here is a Youtube link: https://youtu.be/mkIiOcrxkgM
Vestibulo-ocular reflex gain
Nystagmus and ocular tilt reaction are called static deficits as they occur without patient movement. Changes in VOR gain and defects in vestibulo-spinal tone are dynamic deficits, they occur during movement.
VOR gain is the ratio of eye movement to head movement and the ratio should be 1. This means that, if a patient makes a head movement to the right, their eyes should make an exact equal but opposite to the left. This is how gaze stability is maintained when we are moving. See the vestibular physiology tutorial for more detail.
Following uVD the gain falls and the eyes lag behind the head movement. This means that, during a quick head turn, the eyes will be slow to make equal and opposite movement. Instead they will move in the same direction of the head.
This is easiest to see during a head-thrust manoeuvre. These are used commonly in clinical practice and form the basis of modern vestibular test batteries. The test is also called the head-impulse test and can be done in any of the planes of the semi-circular canals.
Patients experience the loss of gain as a symptom that they describe as being as if the world is catching up with them when they turn. Sometimes they say that it is like their brain lagging behind their head.
Useful fact - changes in gain are asymmetric. The gain difference is greater when turning towards the under-active ear. This means that we can test the semicircular canals separately. For example, turning the head horizontally to the right tests the right lateral canal. If the right canal is under-active the loss of gain will be greater when the impulse is to the right than it will be to the left. This is related to Ewald's second law and to the physiology of the neuroepithelium of the ampulla.
Head Impulse Test
1. Sit opposite the patient and ask them to fix their eyes onto something behind your head (the target).
2. Hold their head between your hands and turn their head quickly to the right by about 20 degrees
3. If the patient has a normal right lateral canal the eyes will remain fixed on the target
4. If the canal is under-active the patient's eyes will jump back to the target and the examiner will see this happen. This is repeatable. The jump is called a re-fixation saccade
5. Repeat the test for the left side
Vestibulo-spinal deficits
The vestibular nuclei generate tonic activity that passes down the vestibulo-spinal tracts in the brainstem and spinal cord, towards anti-gravity muscles and other muscles of posture. Following uVD this tone is reduced or lost and patients say that they drift when they are walking or that they sway.
Early after uVD there is great dependance on visual and somatosensory and proprioceptive information. The brain uses this information to help maintain equilibrium and it will remain important aspects of compensation. Early after uVD, if the environment changes, patient notice a great difference in their equilibrium. For example, walking into a supermarket can cause severe imbalance and seeing movement on a TV or computer screen can be very distressing. Walking in poor lighting situations is also very difficult, for example, at dusk or during the night.
Clinically, we examine for losses in vestibulo-spinal tone by doing the Fukuda step test or Ünterberger test.
Compensation
A useful place to start is with a quotation, 'The term “vestibular compensation” is misleading because it implies a single process and suggests complete recovery. Neither is correct.’ Curthoys and Halmagyi 1995.
In fact there are a number of different processes in play and these work at different rates. For many of these processes recovery is incomplete and deficits can be detected long into the future when examined for appropriately.
The various processes aim to decrease the impact of the static deficits and the dynamic ones and this happens at different rates.
Nystagmus and Ocular Tilt Reaction
Nystagmus undergoes a rapid clinical resolution during the first few days but is still detectable with appropriate electrophysiological testing even a year after uVD. It resolves quickly because of rapid rebalancing of the vestibular nuclei on the two sides. Recall that it is the marked asymmetry in vestibular nucleus activity that is responsible for generating nystagmus.
Ocular tilt reaction will halve by a month but will persist much longer than this.
Compensation for these static deficits occurs in a number of ways:
1. The cerebellum imposes an inhibitory effect on the overactive nucleus (the one that is on the normal side and is not being inhibited in the usual manner). This immediately decreases the imbalance between the two sides and reduces the intensity of symptoms and eases the nystagmus.
2. Receptor sensitivity changes such that the inhibitory fibres from the overactive side have less effect
3. The neurones in the under-active nucleus become intrinsically more excitable
4. Later on there is an expansion in connections with excitatory inputs on the under-active side. This is dependant on the activity of the patient and will further equalise the activity between the two sides
Dynamic deficits also undergo compensation but these are slower and often incomplete. The VOR may never completely recover. Recovery occurs through sensory substitution and behavioural changes. With a weak VOR the patient has the option of blinking during head turning and this reduces the discomfort caused by reduced gain. Using saccades is another strategy. A saccade is a rapid eye movement during which vision is suppressed and these can be used to reduce the unpleasantness of the retinal slip of images during head turning. Behavioural avoidance of provocative movement is another option.
Multi-sensory substitution is the rule if patients are active and engaged with their recovery. There is a critical period after uVD during which the patient should be stimulating their balance system. This is unpleasant for them as it makes them feel sick. They would rather lie still and have vestibular sedatives. However, movement is key to full compensation.
The situation is akin to current thinking about the management of back pain. The sooner you start moving again the more likely that you will recover.
Psychological factors are important too. Motivation, fear of symptoms, anxiety, and prior experience of illness or vertigo can all affect the full recovery of the patient. See the page on PPPD for more information on this.
Decompensation
This is the process by which normal adaptive and behavioural changes are compromised by other events. Vestibular compensation is not a 'one-off' event. It remains a dynamic activity and needs a well functioning brain, body, and psyche to maintain it.
This active compensation can be decreased and the commonest situation that this occurs in is in someone with a strong visual preference in their dynamic recovery. In such patients vision is the dominant sensory substitution following loss of a balance organ. This means that, if the patient's vision is compromised through prescription change, poor lighting, visually active situations such as supermarkets etc, their balance suffers.
Rehabilitation of such patients means focussing on reducing visual dominance and encouraging somatosensory and proprioceptive substitution to some extent.
Rehabilitation of patients who fail to make a good recovery is important and effective.
Close
The loss of afferent information to the vestibular nucleus causes an immediate imbalance in activity within the vestibular nuclei. This is exacerbated by the commissural inhibitory system and nystagmus, ocular tilt reaction, loss of VOR gain and vestibulo-spinal effects are immediate and severe.
Compensation of the loss is a process rather than an event. It is lifelong. It starts quickly, removing the nystagmus and reducing ocular tilt through rebalancing the activity in the two vestibular nuclei via a variety of neural and neurochemical changes. Longterm behavioural adaptations also improve equilibrium but are susceptible to interference for other processes, visual environments, drugs and illnesses.
There are many patients who are unable to make an adequate recovery themselves. Patients with limited mobility, muscular weakness, compromised neurology, and who are on drugs that may be sedating or have disequilibrium as a side effect, may lack the ability to make compensation. For them, rehabilitation through management of their medical complaints, strength and mobility offers a very good chance of improved quality of life.
