1. Name of the location of 90% of epistaxis
2. A genetic disorder that forms AV malformations in the skin, lungs, brain etc
3. Name of posterior vascular plexus in the nasal cavity causing posterior epistaxis
4. 1st line treatment for all epistaxis
5. The common brand name for anterior nasal packing
6. Chemical used in cautery sticks
7. Physically scaring complication of posterior nasal packing with foleys catheter
Coming soon..
Neck Lumps
Neck lumps are fairly common in clinical practice. The underlying diagnosis may be benign or malignant and they commonly arise in lymph nodes, salivary glands, and in the thyroid.
There are a variety of ways of categorising lumps in the neck. Each has its advantages for the student and helps by providing a simple framework upon which to add knowledge. Three common ways to categorise them are: by age, by position in the neck, and whether they are congenital or acquired. Here we will concentrate on their position.
Probably the best way of making a diagnosis is by considering what structures lie under the skin in the anatomical area affected. This requires a little anatomical knowledge. The diagram below shows the important landmarks of the neck.

The neck is divided into anterior and posterior triangles by the sternocleidomastoid muscle. It is important to understand the boundaries of these two triangles as this forms the basis of the physical examination of the neck.

We also divide the neck up into zones as in the following diagram. These are more helpful when describing the position of abnormalities. Each zone has its typical causes for a neck lump.
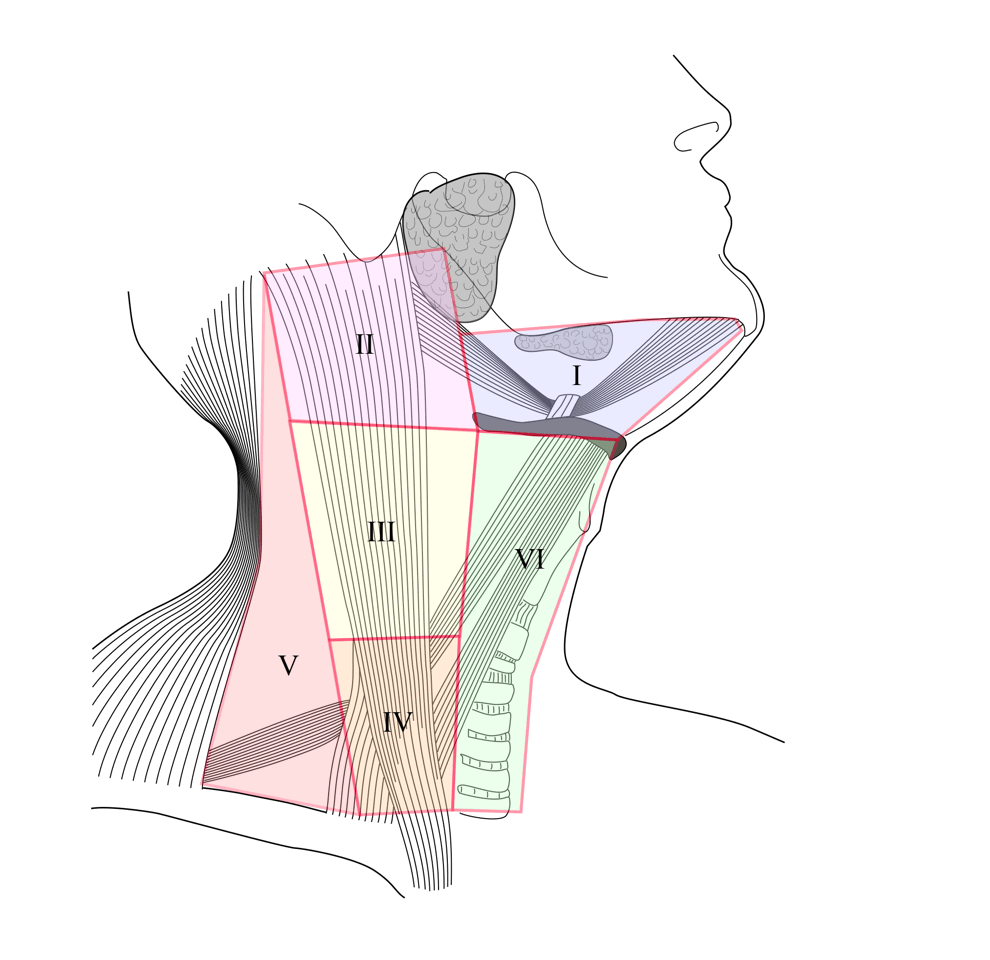
Looking at the levels in the above diagram you can see what pathology might present with a neck swelling. Remember that all levels can have lymph nodes* with inflammatory or malignant disease.
Level I: Submandibular gland tumour *, tooth abscess
Level II: Branchial cyst, parotid tumour *
Level III: Branchial cyst
Level IV: Paraganglioma
Level V: Cystic hygroma
Level VI: Thyroglossal cyst *, thyroid goitre and cyst, dermoid cyst
The important disease for the Swansea ENT syllabus are marked with an asterisk *. These are considered further below. You also need to study thyroid disease as part of your other course requirements.
Benign Lymphadenopathy
By far the commonest cause of a lump in the neck is a lymph node that is reacting to local infection or that has itself become infected. This is especially so in children who, if they have a slim neck, will have palpable nodes for much of their first decade.
They arise secondary to sore throats, tonsillitis, tooth disease, and oral infection. They can arise in of more chronic illnesses too. For example, toxoplasmosis, tuberculosis and atypical mycobacterial infection.
Malignant lymphadenopathy
There is a rule of ‘80’s. 80% of non-thyroid neck lumps in adults are neoplastic and 80% of those are malignant. 90% of neck masses in children are benign.
The corollary to this is that any neck lump in someone over 40 should be considered as a malignancy and investigated appropriately.
Generally, a neck lump caused by a cancer somewhere in the upper aerodigestive tract will be associated with the signs and symptoms of the primary. This means that a neck lump may be accompanied by hoarseness or dysphagia if there is a laryngeal or pharyngeal cancer present.
Students should be aware that there are a set of ‘Red Flags’ for head and neck cancers. These are:
Smoker +/- drinker
Dysphagia
Dysphonia
Haemoptysis
Neck lump
Referred otalgia
Malignant neck lumps are investigated with ultrasound and by fine needle aspiration cytology (FNAC). Chest X-ray is performed because of the risk of secondary spread or a second primary tumour. CT and MRI scanning are also employed for planning of management.
Treatment depends upon the site of the primary tumour. It will include surgery with or without radiotherapy.
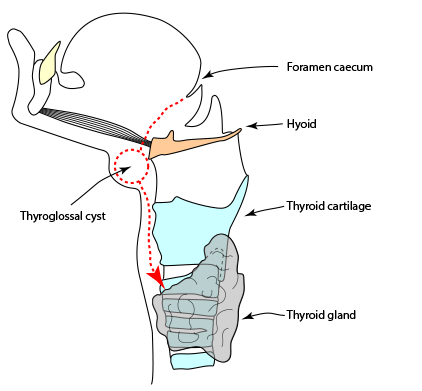
Thyroglossal cyst
This is the most common congenital abnormality causing
a neck lump. It arises when thyroid tissue is left behind
during descent of the thyroid from the tongue base to the
lower neck between the third and seventh week of gestation.
(represented by the red line on the diagram.)
Clinically it presents as a midline lump that moves up on
tongue protrusion and swallowing. This differentiates it
from other midline swellings. Thyroid masses may move
up on swallowing but not on tongue protrusion.
Diagnosis is suspected from the position and physical
findings above and is confirmed with an ultrasound
examination. This scan will show a normal thyroid and the cyst.
Treatment is via excision of the mass plus the middle third of
the hyoid bone with which the cyst is intimately related.
The operation is called a Sistrunk procedure.
Salivary gland tumours
The majority of tumours affecting the salivary glands are in the parotid and are benign. There is an interesting inverse relationship between the size of the salivary gland and the likelihood of the tumour being malignant. Thus parotid tumours are rarely malignant while tumours of the submandibular gland are more commonly malignant. Tumours of minor salivary glands are even more likely to be malignant.
Parotid gland tumours
90% of all salivary tumours affect the parotid and 90% of those are benign. The usual diagnosis is a pleomorphic adenoma (the commonest pathology) or a Warthin’s tumour.
Malignant parotid tumours are uncommon. They are suspected when the mass is fast growing and if there is a lower motor neurone facial nerve weakness associated with the mass. Benign parotid tumours don’t cause facial paralysis.
Investigation of parotid masses is by ultrasound scan and FNAC. Open biopsy is not recommended as it may seed tumour and make future resection difficult. MRI scanning can be used in addition.
Submandibular gland tumours
Although the likelihood of a tumour in the submandibular gland being malignant is greater than in the parotid, tumours here are very uncommon. They present as a mass under the ramus of the jaw and are investigated in the same way as parotid tumours.
Treatment of Salivary Gland Tumours
Benign parotid tumours are removed by a superficial parotidectomy as the tumours are almost always in the superficial lobe. Care is taken not to damage the facial nerve within the gland.
Benign tumours of the submandibular gland are excised. The nerves to avoid here are the marginal mandibular branch of the facial nerve, the hypoglossal nerve and the lingual nerve.
Malignant tumours are managed in the context of a multidisciplinary team. They are excised taking care to preserve the regional nerves. Elective dissection of the neck is often performed to clear lymph nodes that may harbour microscopic metastases. Adjuvant radiotherapy is considered in more aggressive tumours.
A patient comes to you with a neck lump...
Begin with a history. How old is the patient, how long has it been there, what other symptoms does the patient have, and do they smoke or drink? Concentrate particularly on red-flag type symptoms of dysphagia, dysphonia, coughing up blood, and referred ear pain.
Examination will reveal a lot about the underlying pathology. Where is the lump, is it mobile or tethered, is it hard, soft or rubbery, is there tenderness, fluctuation, or a vascular thrill? Does it move on swallowing or tongue protrusion? Does it change size with eating?
Ultrasound scanning with or without fine needle aspiration cytology will almost always give a diagnosis so a referral is required. A chest X-ray may be required depending on the history and presence of smoking, and MRI or CT scanning are used to stage malignant disease.
Take a short assessment to test your knowledge here.
Appendix (alternative ways of classifying neck lumps)
By location
By age
These age ranges are not infallible and are meant only as a guide.

