1. Name of the location of 90% of epistaxis
2. A genetic disorder that forms AV malformations in the skin, lungs, brain etc
3. Name of posterior vascular plexus in the nasal cavity causing posterior epistaxis
4. 1st line treatment for all epistaxis
5. The common brand name for anterior nasal packing
6. Chemical used in cautery sticks
7. Physically scaring complication of posterior nasal packing with foleys catheter
Coming soon..
Epistaxis
Objectives
1. Be aware of the structure and function of the normal nose and sinuses with particular reference to the following:
- External nose
- Nasal cavity and paranasal sinuses
Have an awareness of how these structures change when affected by disease and understand how this
leads to dysfunction and patient morbidity and mortality.
2. Understand the incidence/prevalence, clinical presentation, the management and prognosis of epistaxis.
Definition
“Epistaxis is the medical term for a nosebleed. The commonest reason for emergency admission to the ENT ward.”
Prevalence
~ 60% of the population in a lifetime
~ 6% require medical intervention
Mostly ages 2 -10 & 50 - 80
Potentially fatal!
Aetiology
The causes of epistaxis can be broadly split into two categories:
- Local
- General (systemic)
Rhinosinusitis
Commonest cause 85%
Inflammatory
Idiopathic
Blow to face
Local
Neoplastic
(rare)
Traumatic
Nose picking
Iatrogenic
Nasal sprays
Post surgery
Hereditary telangiectasia
Hereditary
Primary
Platelet disorders
General
Primary
Secondary to drugs
e.g. aspirin / clopidogrel
Bleeding diathesis
Secondary to drugs
e.g. warfarin
Clinical relevance
Hypertension does not cause epistaxis, however, it prolongs bleeding when established.
Anatomy of the nose
Here we will review the vasculature of the nasal cavity. For a more in depth of the look at the anatomy of the nose please see the nasal anatomy tutorial.
The nasal cavity has a rich and complex blood supply that makes it ideally suited for its function of warming inspired air. The crux of this adaptation is seen when disruption of this complex network of vessels causes epistaxis.
The diagram below shows clearly the nasal septum is supplied by 5 main arteries.
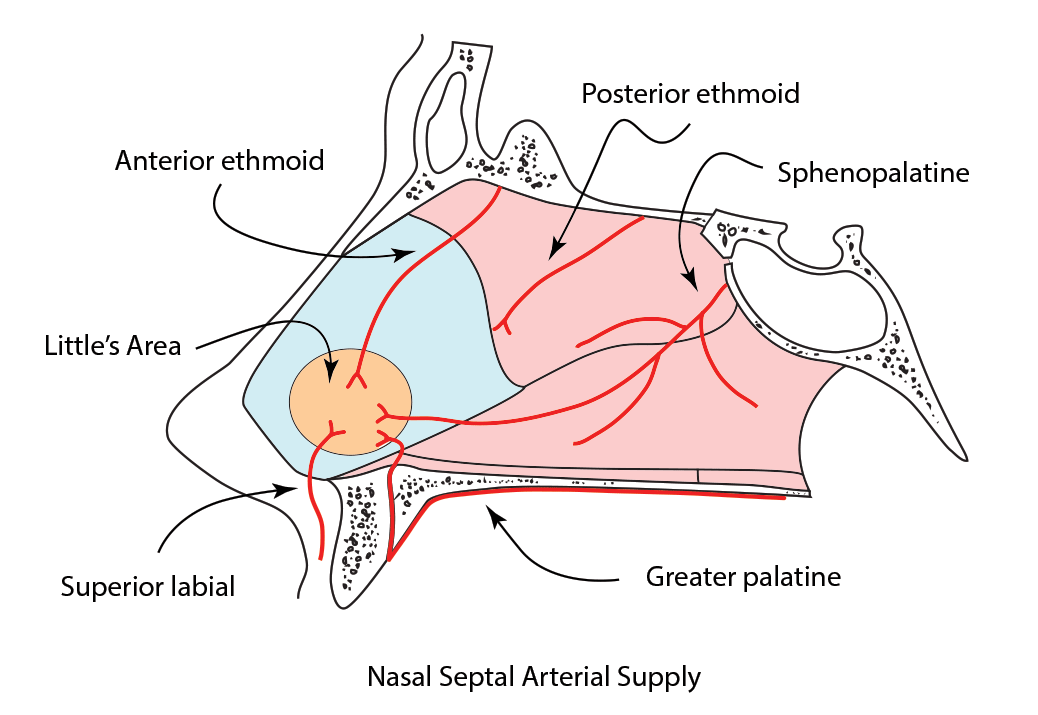
The vessels anastomose to form a network of vessels on the anterior nasal septum called Little's area (Kiesselbach plexus). This is the most common bleeding site seen in 90% of anterior bleeds.
There is a second site of anastomosis seen on the posterior nasal septum called Woodruff's plexus.
Epistaxis can be broadly categorised into two main types depending on the location of the bleeding vessel.

Younger
Easier to manage
90% from Little's area
Blood from one nostril when head tilted forward
Posterior
Older
More difficult to manage
More dangerous
Woodruff's plexus
Blood passes down post nasally, oropharynx, often both nostrils anteriorly
Anterior
Management
The management of epistaxis should be tackled with a methodical, stepped approach. The algorithm below summarises this approach nicely.
Epistaxis management Algorithm
Step 1
Step 2
Assessment of the patient with ATLS principles, ABCD approach, patient resuscitation
Simple first aid
“15 minutes of uninterrupted pressure on soft part of nose with head tilted forward”
Step 3
Step 4
Examination of the nasal cavity. Identify bleeding point
Silver nitrate / electric cautery
Haemostasis achieved?
YES
NO
Step 5
Patient discharged with naseptin nasal cream 2/52.
Insertion of anterior nasal
packing
Step 6
Haemostasis achieved?
YES
NO
Pack removed after 24 hours
Repeat from step 2
Posterior pack insertion +/- theatre
Nasal Cautery
Nasal cautery is the process of sealing the bleeding vessels and can be conducted in a number of ways. There are two main methods commonly used by most ENT departments
1. Silver nitrate (cautery sticks)
A small plastic stick with silver nitrate on the end that reacts when in contact with the moist
nasal mucosa. AgNO3 + H20 --> AgOH + HNO3 (Nitric acid)
2. Electrocautery (specialist ENT department)
Usually conducted in an operating theatre.
-
Bipolar
-
Monopolar
Cautery should not be conducted bilaterally as this will damage the blood supply to the cartilaginous nasal septal resulting in a perforation.
If both sides of the nose need cautery, as is often the case in young children, cauterise the worse side first and then cauterise the second side a few weeks later.
The three images below illustrate cautery of an anterior epistaxis.

This is the left Little's area. A rich anastomosis is seen.

Silver nitrate cautery is applied to the periphery of the anastomosis first. It leaves a small grey chemical burn over the vessel which denatures protein and causes occlusion of the blood vessel and eventual scarring.

Cautery progresses so that all the vessels are touched. Generally one starts with the smaller ones and work towards the largest.
Cautery procedural video
Anterior nasal packing
Nasal packing is placed when simple haemostasis measures fails. Packs come in a variety of different shapes, sizes and include some that inflate with water and others that inflate with air.
All packs work on the theory of creating a pressure tamponade on the bleeding vessels.
Placement method
The pack is inserted horizontally into the affected nostril.
(Parallel to the nasal floor)
Air or H20 is used to inflate the pack
The pack is left in situ for 24 hours to allow clot formation.
If haemostasis fails then a pack can be inserted into the contralateral nostril to tamponade the septum.
In persistent bleeding, a posterior pack can be inserted.

Anterior nasal packing procedural video
Clinical Note
If a pack is in for >24hrs then prophylactic antibiotics are given to prevent infection in the nose, sinuses or middle ear.
Posterior nasal packing
For posterior epistaxis in which an anterior nasal pack has failed to achieve haemostasis, a posterior pack can be inserted to halt the bleed.
As for anterior nasal packing if haemostasis is not achieved with a single pack, a second pack can be inserted into the collateral nostril to tamponade the septum and completely pack the nasal cavity.
Placement method
A Size 14fg Foley catheter is inserted into the nostril and advanced until visualised in the oropharynx.
The balloon is inflated with 10ml of sterile water to occlude the choana.
The anterior nasal cavity is packed, the pack inflated and a clamp holds the catheter in place.
The clamp is regularly rotated and gauze is used to protect from alar (pressure) necrosis.
Posterior packs are often left for 24 hours, as a temporary measure to buy time before the patient is taken to theatre.

Clinical Note
Alar necrosis has a massive cosmetic impact, causing unsightly scarring. There are medicolegal implications!
Posterior nasal packing procedural video
Surgical management
Surgical management is a last resort for patients who have failed to achieve haemostasis with conservative management. As with all treatments a stepped approach is advised with many patients requiring simple measures in the controlled theatre environment. Other patients require higher risk procedures when all else has failed. The list below summarises this stepped approach, with a patient moving onto the next more invasive procedure if haemostasis fails with the attempted method.
-
Examination under anaesthetic
-
Electrocautery
-
Vessel ligation (e.g. SPA)
-
Embolisation
-
Ligation of external carotid
Increasingly invasive procedure
Test your knowledge in a self-assessment quiz here
Alternatively, why not try out our epistaxis podcast
20 minutes to spare? Why not try our epistaxis Kahoot!
